Hypertension (defined as blood pressure of 140/90 mmHg) is an extremely common co-morbid condition in diabetes, affecting approximately 20-60% of the individuals with diabetes. It complicates diabetes in all populations and occurs with increasing frequency with advancing age. Both disorders are potent independent risk factors for cardiovascular, cerebral, renal, and peripheral atherosclerotic vascular disease. The prevalence of hypertension is 1.52.0 times more in those with diabetes than in those without diabetes. Hypertension is more prevalent in diabetic men than diabetic women below 50 years of age and more common in women thereafter. Risk factors for hypertension in most countries are diabetes mellitus, obesity, sedentary behaviour, alcohol, higher social class, salt intake and smoking.
Complications
Hypertension is a major contributor to morbidity and mortality in diabetes than normotensive diabetic individuals and hence should be recognised and treated early and aggressively. It has been clearly shown that hypertension in diabetic patients is associated with accelerated progression of both microvascular (retinopathy and nephropathy) and macrovascular (atherosclerotic) complications (Table 1).
Management Strategies
Usually, the management of the hypertensive diabetic patient involves a three-prong approach:
- control of blood pressure
- control of glucose and
- control of lipids.
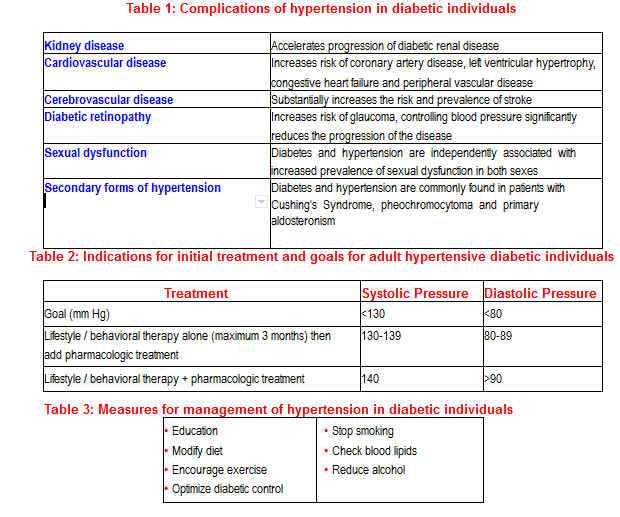
To summarise, a hypertensive individual with diabetes should therefore be treated with the appropriate behavioral therapy and antihypertensive drugs and be carefully monitored to ensure satisfactory blood pressure control and prevention of end-organ complications.




4 thoughts on “Diabetes and Hypertension”
Diabetic 200 after meals
Diabetic 200 after meals