Insulin Management
Understanding Insulin Management
Based on the type of diabetes and the level of sugar control, certain patients may be suggested to start insulin treatment. In addition to timely initiation, regular adjustment of insulin doses based on the sugar levels is critical for improving glycemic control and preventing diabetes-related complications.
Based on the pattern of sugar levels, different insulin regimen can be used. The various types of insulin available today differ in their onset and duration of action as well as the cost. The expert diabetes consultants at Dr Mohan’s Diabetes Specialities Centre are at hand to help patients choose the best possible insulin regimens for their glucose profile and lifestyle- a perfect example of the personalized care that we offer.
In certain patients. The Continuous Subcutaneous Insulin Infusion pump (CSII) may be an attractive alternative to multiple daily insulin injections. At Dr Mohan’s Diabetes Specialities Centre, we provide patients with the latest information regarding the insulin pump and other recent advances in the field and also provide education and training to help them make the best possible use of these technologies.
INSULIN PUMP THERAPY
Insulin pumps have been shown to improve glucose control for patients who are on multiple doses of insulin and it can provide a better quality of life. An insulin pump delivers a small amount of insulin continuously around the clock. This can lead to major improvements in blood glucose control and offers a higher standard in diabetes management.
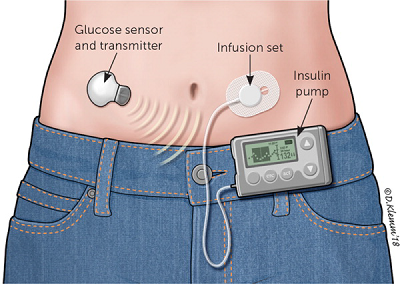
An insulin pump is a small, battery-operated device about the size of a pager that can replace insulin injections of patients managing diabetes. The insulin pump has a small cartridge called a “reservoir” which holds the insulin. The pump uses an infusion set with a tiny, soft plastic tube called “cannula”. The end of the cannula comfortably lies just beneath the skin. The infusion set is generally replaced every 2 to 3 days. The pump can be comfortably disconnected from the body during the shower, change of clothes or while playing sports. The insulin pump is easy and discreet to wear. The pump can be attached to the belt or placed in the pocket or under the clothing.
The insulin pump delivers insulin as “basal” and “bolus” doses.
A small amount of regular or rapid-acting insulin is delivered continuously over a period of 24 hours. This helps to maintain the blood glucose levels within normal limits between meals and overnight. The pump can be adjusted for different basal insulin infusion rates at different times of the day, closely mimicking a healthy pancreas.
The bolus dose is an additional insulin dose delivered to cover meals or to correct high blood glucose.
- Insulin pump helps in better glycemic control –It almost mimics the secretion of insulin from the normal pancreas and helps in a tighter control of diabetes which helps to prevent complications.
- Insulin pump therapy helps patients to prevent:
1) Hyperglycemia (high blood sugar), which can degrade health over time and lead to complications of diabetes
2) Hypoglycemia (low blood sugar), an acute condition that can be very dangerous, particularly at night while a patient sleeps. - The pump is precise and accurate –it delivers insulin precisely and accurately in 0.05 unit increments, which is practically impossible when using traditional injection therapy.
- More flexibility in lifestyle – The patient can adjust or stop insulin delivery for exercise or other needs. Patients with injection therapy have to follow rigid schedules of insulin shots, meals and snacks but patients using an insulin pump can program insulin delivery based on when and what they eat. Therefore, life is more flexible with insulin pump therapy.
An insulin pump is an excellent tool for helping people to improve glycemic control. Numerous studies have shown that more patients who are on insulin pump therapy achieve their target HBA1C than those with traditional insulin injections. This will help them prevent long-term complications of diabetes.
Frequently Asked Questions
- Sugar, honey, glucose, jam, jaggery, sweets, cakes.
- Dry fruits like dates, raisins, figs
- High calorie fruits like banana, mango, jack fruits, chikku, custard apple, grapes.
- Tender coconut water, soft drinks, beverages
- Bakery products
- Getting rid of trash, salt, and excess water in your body
- Keeping your body’s fluid balance in check
- Assisting with the regulation of your blood pressure
Eat the Right Carbs(carbohydrate) and high fibre foods Carbohydrates are an essential source of energy, fibre and micronutrients. Carbohydrates are present in
- cereals like rice, wheat, ragi, bread, pasta etc
- starchy vegetables like potatoes, yam colcasia
- fruits, sweets, sugar and dairy products
Foods that contain little or no carbohydrates include meats, poultry, fish, egg, non starchy vegetables and fats.Carbohydrates get converted into blood glucose quickly and thereby increase the blood glucose level. Therefore the quantity and quality of carbohydrate consumed is important. Hence it is essential to choose low carbohydrate foods .
It is better to prefer complex carbohydrates and high fiber foods like whole grains, whole pulses and non starchy vegetables as it delays digestion and helps for a better glycemic control.
Choose low glycemic index foods
Glycemic index(GI) is a value assigned to foods based on how slowly or how quickly a food raises the blood glucose levels. The GI is not related to whether the carbohydrate is simple or complex. The GI measures the rise in blood glucose levels caused by a measured quantity of a particular food. Carbohydrates in low GI foods gets metabolised slowly and cause a lower and slower rise in blood glucose levels. High GI foods are rapidly absorbed and cause a large rise in blood glucose levels. Examples of low, medium and high GI foods are as follows
- Low GI: Greens and Green leafy vegetables
- Moderate GI: Whole grains, Brown rice, Legumes, Dhals, Dr.Mohan’s Brown rice, Dr.Mohan’s High fibre rice etc
- High GI: White fully polished rice, Sugar, Jaggery, White bread, Maida etc
Follow a Healthy Diet
Diabetes control depends to a great extent on following the right/ healthy diet. Knowing what to eat and what not to eat is extremely important. Healthy diet helps to prevent wide fluctuations of blood glucose levels .Diabetic diet does not mean that one has to starve or have a bland diet. You can enjoy your favourite foods and take pleasure from meals without feeling hungry or deprived.To eat healthy
- Eat 4 meals (Breakfast, Lunch, Evening snack & Dinner) a day
- Eat at the same time every day
- Eat the right quantity of food
- Eat more vegetables
- Eat less fat and salt
The key point is that people with diabetes do not need a special food. Learn to watch on portion sizes and do not eat high calorie foods
Dietary fibre is a type of carbohydrate that is found in plant-based foods. It is not absorbed or digested by the body,but plays an important role in maintaining good health. There are two types of dietary fibre – soluble fibre and insoluble fibre
- Soluble fibre- found in fruits and vegetables
- Insoluble fibre- found is whole grains and whole pulses.
- Fibre is not digested or absorbed like other starches, it slows the absorption of sugar and has less of an effect on increasing blood glucose levels
- Fibre helps to improve insulin sensitivity
- Foods high in soluble fibre plays a major role in reducing blood cholesterol and low-density lipoprotein, or “bad,” cholesterol levels
- Having diabetes can increase the risk of cardiovascular disease. Evidence shows that increasing the intake of fibre, especially whole grains help to reduce the risk of cardio-metabolic diseases (this includes cardiovascular disease, insulin resistance and obesity) and colo-rectal cancer
- Dietary fibre absorbs fluid and increases the bulk of waste matter, making the stools softer and easier to pass
- Increasing dietary fibre also helps to promote weight loss and maintenance.High-fibre foods tend to be more filling than low-fiber foods. A high-fiber food tends to take longer time to eat and to be less “energy dense,” which means the calories are less for the same volume of food.
It prevents blood sugar fluctuations
Individuals with diabetes may be on tablets or insulin or both. Hence it is essential to follow a 4 meal pattern to prevent wide fluctuations of blood glucose. This will also help in reducing the next meal portion
Small frequent meals help to control the portion size of each meal. On contrary if any of these meals are missed or skipped it increases the appetite and leads one to consume a large portion size for the following meal
Fill half of your plate with vegetables and greens, one fourth with whole grams and pulses (if non-vegetarian pulses & non-vegetarian food) and the remaining one fourth with cereals (whole grains) like unpolished/minimally polished rice, Dr.Mohan’s brown rice, high fibre rice or wheat. Watch your portion sizes.
- Follow the medicines as suggested by your Diabetologist
- Do not stop insulin or try any alternative treatment
- Self-monitor your blood glucose levels
- Have a periodic review and keep adjusting your insulin
- Follow the diet as suggested by your Dietitian
- Do not restrict your physical activity
- Do not look this as a social stigma. Sharing experiences is a powerful way to learn to manage diabetes hence talk to other persons with a similar disorder. The diabetes care team is there to help meet all your medical needs and support
- You spend almost 35 hours per week at your school, so managing diabetes at school is very important.Fluctuations of blood sugars can affect the ability to learn. Hence it IS important that school staffs are educated, equipped and available to support the child
Many schools have little experience caring for a student with diabetes and may not know what is involved in diabetes management. It will take some time for the school to get used to caring for your child, just as it took some time for the child’s parents and the child as well.Talk to the school administrators and all staff members about what diabetes means for the child.Make sure the child always has everything required to manage diabetes at school.
- Healthy snack
- Glucose tablets
- 2 juice boxes (up to 15g of carbohydrates)
- Share helpful information about diabetes with school personnel.
- Link the school to a diabetes educator who can help to train and educate teachers and other school personnel about diabetes.
- Discuss the Diabetes Medical Management Plan provided by your child’s health care provider and work together to develop a plan for school including:
- Blood glucose checks
- Insulin administration
- Snacks and meals
- Emergency situations or when glucagon is needed
- Describe the child’s usual symptoms of hypoglycemia and hyperglycemia. Provide updated phone numbers. Develop a plan for when you should be called.
- Talk about what to do in an emergency. Make sure a trained school staff member know when and how to manage hypoglycemia.
- Provide diabetes management materials and equipment that should be kept at school.
- Work together with friends and school administrators to gather and distribute training information
