“SICK DAY RULES”
What happens when people living with diabetes are ill?
When people living with diabetes are ill, their bodies react by releasing hormones to fight the illness. These hormones can be triggered by any number of conditions, such as infections, cardiovascular ischaemic events, gastroenteritis, dehydration etc. The hormones released during an illness raise blood sugar levels and at the same time make it more difficult for insulin to lower them. For people living with diabetes, even a minor illness can lead to dangerously high blood sugar levels. This may cause life-threatening complications, such as diabetic ketoacidosis or a hyperosmolar hyperglycaemic state.
Illnesses most likely to have an effect on blood glucose levels:
– Common cold or flu, including COVID-19
– Sore throat
– Urinary tract infections
– Bronchitis or chest infections, Stomach upsets and diarrhea
– Skin infections such as abscesses (especially if these conditions are followed by a fever or high temperature) Starting a course of cortisol, or increasing the amount of cortisol taken, also has a significant impact on blood sugar levels.
Ketoacidosis symptoms:
− Blood glucose over 15 mmol/l (270 mg/dl)
− Ketones in urine
− Thirst
Seek urgent help if:
− Vomiting
− Rapid breathing with fruity-smelling breath
− Abdominal pain
− Reduced level of consciousness (drowsiness)
Planning ahead
People living with diabetes, their carers, and parents of children living with diabetes should work with their healthcare team to make an illness plan. They should discuss:
– their target blood sugar goal during an illness
– how to adjust their medicines (for example how to adjust their insulin dosage and when to take insulin)
– when to contact their healthcare team for help
– how often to check their blood sugar and ketone levels.
When ill, extra insulin might be necessary as blood glucose levels may rise even if patients are unable to eat or drink normally.
When to contact a doctor?
People living with diabetes should contact their healthcare team:
– If they are not sure what to do
– If they vomit repeatedly (not able to hold down any food or drink for more than six hours), as they can quickly become very dehydrated
– If their blood glucose stays high for more than 24 hours
– If they develop symptoms which could be indicative of their developing diabetic ketoacidosis
General guidelines to manage diabetes during an illness
If a person with diabetes becomes ill, the following steps should be followed, even if the blood sugar levels are
within the target range:
- Take diabetes medication as usual. Insulin treatment should never be stopped
- Test blood glucose every four hours, and keep track of the results
- Drink extra (calorie-free) fluid*, and try to eat as normal
- Weigh yourself every day. Losing weight while eating normally is a sign of high blood glucose
- Check temperature every morning and evening. A fever may be a sign of infection
*Drink plenty of fluids – 120 to 180 ml every half an hour to prevent dehydration. It might also be necessary to drink sugary beverages if it is not possible to take in 50 grams of carbohydrates through food. The amount of sugary beverages should nevertheless be carefully controlled to prevent blood sugar levels from rising too much.
Guidelines for People with Type 1 Diabetes
During a period of illness:
- Insulin treatment should never be stopped
- The insulin dose may need to be increased and it might be necessary to take additional doses of
- Fast-acting insulin to bring down the blood sugar levels
- Blood glucose levels should be checked at least every four hours
- Plenty of non-sweet fluids should be drunk to avoid dehydration
- Ideal blood sugar levels should be between 6-10mmol/l (110-180 mg/dl)
If the blood sugar levels are in the following ranges at any time:
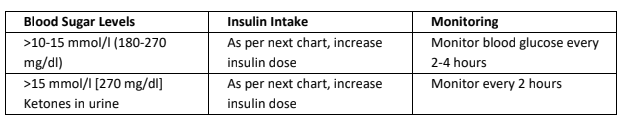
Everyone with T1D should have test strips for monitoring blood sugar at home and, if possible, also blood ketone strips and urine strips to test for ketones during illness and other times when the blood glucose levels are high. If the test is positive for ketones, then hospital treatment should be sought.
Recommendations for insulin adjustment for people with T1D on basal bolus treatment
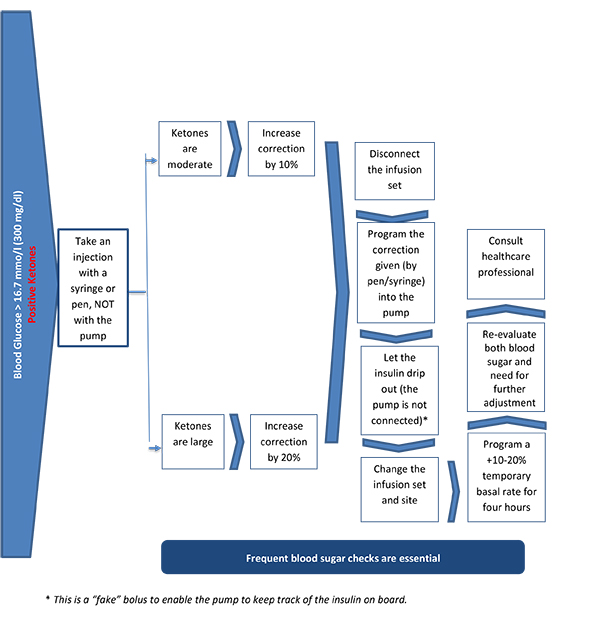
- Test blood sugar levels and ketones (especially if blood sugar >15 mmol/l [270 mg/dl]) every four hours, day and night. If blood ketones are >3.0 mmol/l at any time, go to the hospital immediately; intravenous (IV) insulin and fluids might be required.
- The Total Daily Dose (TDD) formula helps to decide how much extra rapid or fast-acting insulin a person needs to take.
- Add up the number of units of insulin (all kinds) that the person usually takes each day. (Use baseline or usual doses). The TDD =_ units.
- Calculate 10% = 15% = __20% = of TDD. This is the extra dose (or supplement).
- Follow the chart below to decide how much fast/rapid acting insulin to take every four hours, in addition to the usual baseline insulin doses. Repeat insulin every four hours, if needed, as per the chart below.
- If not eating as usual, replace the usual carbohydrates with sugar-containing fluids.
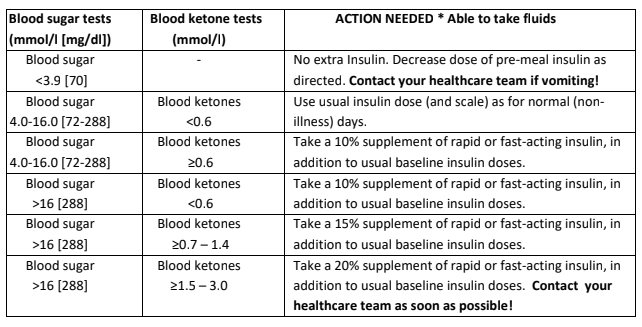
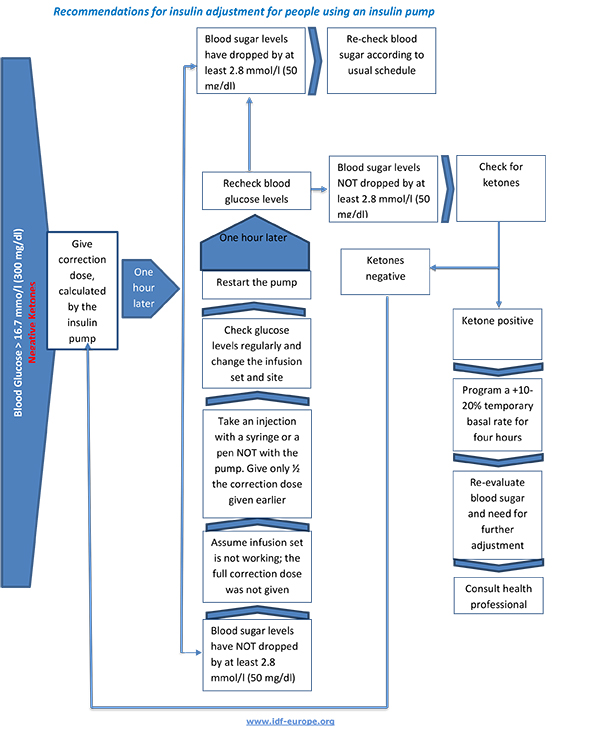
Guidelines for people living with Type 2 Diabetes
People with Type 2 Diabetes should check whether they develop the following symptoms which may be indicative of high blood sugar levels:
– Thirst/dry mouth
– Passing large amounts or urine (this can lead to dehydration)
– Tiredness
– Weight Loss
Guidelines for people with Type 2 Diabetes on tablets:
If a person with T2D takes metformin tablets, it may be necessary to temporarily stop these tablets. This is usually advised if the person has a severe infection or becomes dehydrated.
If it is necessary to stop taking metformin, then an alternative treatment needs to be put in place until the metformin treatment can be resumed (this may include other anti-diabetic pills or even insulin sometimes, depending on the individual levels of blood sugar rise).
People on other oral diabetes treatment may have been provided with blood glucose testing equipment to ensure that their blood glucose levels do not fall too low (hypoglycaemia) and to routinely monitor their diabetes. For those people, there is no need to test very often. During an illness, blood glucose levels usually rise. People with T2D should use the test results as a guide and aim to keep their blood glucose levels between 6 and 10 mmol/l (110 and 180 mg/dl). They may need to test their blood glucose levels at least twice a day.
Guidelines for people with Type 2 Diabetes on insulin:
People with Type 2 diabetes on insulin must be provided with the equipment needed to test their own blood glucose levels at home. The aim should be to keep blood glucose levels between 6 and 10 mmol/l [110 and 180 mg/dl].
- If the blood glucose levels stay above 10 mmol/l (180 mg/dl), they should increase their insulin dose. Extra blood glucose testing will often be necessary. Testing should be done every four hours, especially if the blood glucose levels are high (over 15 mmol/l [270 mg/dl]).
- Ketones: If the blood glucose levels get too high (over 15 mmol/l [270 mg/dl]), then they may need to perform a urine test for ketones. If it is positive, they should contact their health-care provider for advice.
STAY SAFE, KNOW AND APPLY THE SICK DAY RULES!