Mucormycosis in Diabetes
Rhino-orbito-cerebral mucormycosis is an uncommon but serious fungal infection with high morbidity and mortality, caused by the angiotropic fungus. Mucormycosis has suddenly become a household term, causing great fear and panic during this second wave of COVID pandemic in India.
It usually occurs in immunocompromised individuals including people with uncontrolled diabetes, hematologic cancers, HIV/ AIDS, those with solid organ transplants or stem cell transplants and those on immunosuppressants like steroids.
The suspicion or diagnosis of rhino-orbital cerebral mucormycosis triggers a medical as well as surgical emergency with special stress on the need for interaction and coordination among the inter-professional team to improve treatment outcomes in this life-threatening disease.
Who is predisposed/ at risk?
- Uncontrolled diabetes
- Immuno-suppression with steroids
- Treated for Covid-19 with immunomodulators or steroids
- Other comorbidities like malignancy, post-transplant
- Prolonged stay in ICU
- On mechanical ventilation/oxygen therapy for a long period
- HIV/ AIDS
Symptoms
- Facial pain/ cheekbone pain/ toothache
- Sinus headache
- Stuffy nose
- Blood discharge from nose
- Redness of the eyes
- Double vision/ blurry vision/ sudden loss of vision
Signs
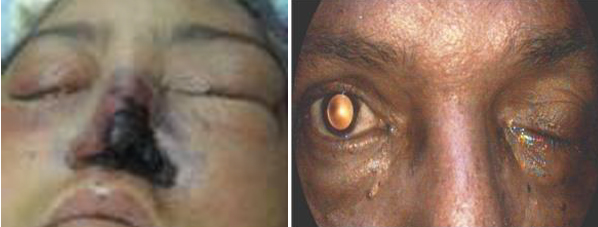
- Facial swelling/ discoloration
- Palatal eschar/ Nasal Eschar (blackish material)
- Ptosis (drooping of the eyelid)
- Proptosis (protrusion of eye)
- Ophthalmoplegia (paralysis of eye muscles) / Restricted extraocular movements
- Pan-ophthalmitis
- Central Retinal Artery Occlusion (CRAO) with a cherry-red spot at the macula
Do’s to prevent
- Control blood sugar level
- Judicious use of steroids
- Monitoring of blood glucose post-Covid-19 in individuals with and without diabetes
- Use of sterile water for humidifiers –while on oxygen therapy
- Watch for early warning symptoms/ signs
Wear a clean mask and maintain personal hygiene
Dont’s
- Do not use any medications like steroids or antifungal agents without consulting a physician
- Don’t waste crucial time. Consulting your diabetologist / ENT doctor or Eye doctor immediately is essential.
Investigations
- Haemogram
- Fasting / post-prandial blood glucose levels, HbA1c
- Renal function tests
- CT scan of Paranasal sinuses
- MRI scan of Brain and orbit
- Deep nasal swab/sputum examination
- Diagnostic nasal endoscopy/ broncho-alveolar lavage
Management
- Urgent medical and surgical management by a team approach involving the Diabetologist, ENT specialist, Ophthalmologist, Intensivist, Maxillo-facial surgeon, Microbiologist and Neurologist.
- Tight control of blood glucose levels and management of diabetic ketoacidosis (DKA). DKA if present, will mostly need insulin for control.
- Increase frequency of self-monitoring of blood glucose by glucometer. If possible, use continuous glucose monitoring by wearing a sensor.
- If a patient is still on steroids, reduce the dose and discontinue it as soon as possible.
- To discontinue the immunomodulatory drugs, if the patient is on any.
- Proper guidelines of anti-fungal therapy like Amphotericin B or others.
- Extensive surgical debridement when indicated.




